When it comes to managing sleep apnoea, Continuous Positive Airway Pressure (CPAP) machines have emerged as one of the most effective treatments. For those in Australia, the process of selecting the right CPAP machine can seem daunting, given the myriad of options available. This article aims to provide insights into what to consider when purchasing a CPAP machine, ensuring that you make an informed decision tailored to your specific needs.
Understanding CPAP Machines
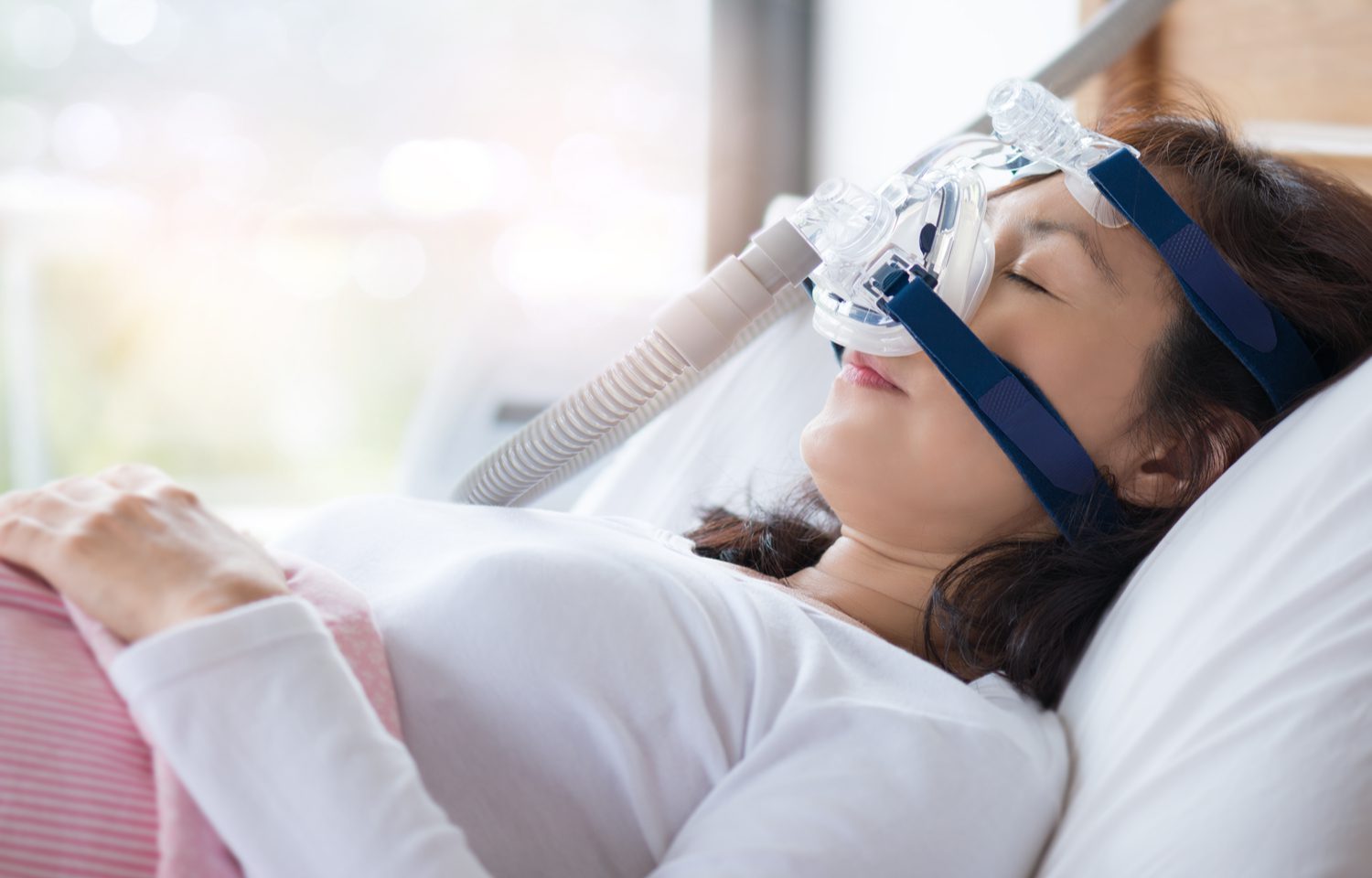
CPAP machines work by delivering a steady stream of air through a mask, keeping the airways open during sleep. This prevents the interruptions in breathing that characterise sleep apnoea. While the fundamental function of these devices remains the same, various models and features can significantly impact user experience and effectiveness.
Choosing the right CPAP machine Australia involves careful consideration of various factors, including the type of machine, comfort and fit of the mask, portability, and budget. By understanding your needs and exploring the options available, you can make an informed decision that enhances your sleep quality and overall well-being.
Types of CPAP Machines
There are several types of CPAP machines available, each designed to cater to different needs. The most common types include standard CPAP, Auto-CPAP (APAP), and BiPAP machines. Standard CPAP machines deliver a fixed pressure throughout the night, while Auto-CPAP machines adjust the pressure based on the user’s breathing patterns. BiPAP machines, on the other hand, provide two levels of pressure: a higher pressure for inhalation and a lower pressure for exhalation.
Understanding these differences is crucial. For instance, those who experience varying levels of obstruction may benefit from an Auto-CPAP, whereas individuals who struggle with exhalation may find BiPAP machines more comfortable. Consulting with a healthcare professional can help determine which type is best suited to your condition. It is also worth noting that some machines come equipped with advanced features such as integrated wireless connectivity, allowing users to track their sleep data and share it with healthcare providers. This can lead to more tailored adjustments in treatment, enhancing overall effectiveness.

Key Features to Consider
When selecting a CPAP machine, several features can enhance your experience. Humidifiers, for instance, are a common addition that can alleviate dryness and irritation in the airways. Many modern machines come with built-in humidifiers, while others offer them as optional attachments.
Another important feature is the noise level of the machine. A quieter unit can significantly improve sleep quality for both the user and their partner. Additionally, consider the size and weight of the machine, especially if you plan to travel with it. Compact and lightweight models are available, making them easier to transport. Furthermore, some CPAP machines now include smart technology that can automatically adjust settings based on environmental factors such as altitude and humidity, ensuring optimal comfort no matter where you are. This level of adaptability can be particularly beneficial for frequent travellers or those living in areas with fluctuating weather conditions.
Comfort and Fit of the Mask
The mask is arguably the most critical component of a CPAP machine. A well-fitting mask ensures effective therapy and enhances comfort during use. There are various types of masks available, including nasal masks, full-face masks, and nasal pillows. Each type has its own advantages and disadvantages, and the choice largely depends on personal preference and comfort.
Learn more on: How CPAP Machines Improve Sleep Quality for People With Apnoea
Choosing the Right Mask Type
Nasal masks cover the nose and are often preferred for their minimalistic design. They are suitable for those who breathe through their nose and do not require high pressure settings. Full-face masks, on the other hand, cover both the nose and mouth, making them ideal for mouth breathers or those who require higher pressure. Nasal pillows provide a more unobtrusive option, delivering air directly into the nostrils.
It is essential to try on different masks to find the best fit. Many suppliers offer fitting services or trials, allowing users to test various options before making a commitment. A proper fit not only enhances comfort but also ensures effective therapy by preventing air leaks. Additionally, the material of the mask plays a significant role in comfort; soft silicone or gel cushions can reduce irritation and pressure marks on the skin, making it easier to wear the mask throughout the night. Learn more about irritation on https://www.dermcoll.edu.au/atoz/irritant-contact-dermatitis-icd/
Adjustability and Customisation
Many modern CPAP machines offer adjustable settings that allow users to customise their therapy. This includes pressure settings, ramp features that gradually increase pressure, and even smart technology that tracks usage and sleep patterns. These customisable features can significantly enhance the user experience and improve adherence to therapy.
Furthermore, consider machines with user-friendly interfaces. A clear display and intuitive controls can make it easier to adjust settings and monitor usage, contributing to a more satisfying experience overall. Some devices even come with companion apps that provide insights into sleep quality and therapy effectiveness, allowing users to make informed adjustments. This level of engagement can empower individuals to take control of their sleep health, fostering a proactive approach to their CPAP therapy.
Moreover, the importance of regular maintenance cannot be overstated. Keeping the mask clean and replacing components as needed can prevent discomfort and ensure optimal performance. Many users find that establishing a routine for cleaning their equipment not only prolongs the life of the mask but also enhances their overall experience, leading to better adherence to therapy. Regularly checking for wear and tear can help users identify when it’s time for a replacement, ensuring that they continue to receive the best possible treatment for their sleep apnea.
Portability and Travel Considerations
For those who travel frequently, portability is a vital consideration when selecting a CPAP machine. Many manufacturers now offer travel-friendly models that are compact and lightweight, often with travel cases included. These machines can be easily packed and taken on trips, ensuring that therapy continues uninterrupted.
Power Options for Travel
When travelling, it’s essential to consider the power options available for your CPAP machine. Some models come with battery packs or can operate on 12V power sources, making them suitable for use in cars or on camping trips. This flexibility can be a significant advantage for those who are often on the move.
Additionally, check whether the machine is compatible with international voltage standards if you plan to travel overseas. Some devices come with universal power supplies, while others may require a voltage converter.
Accessories and Maintenance
CPAP machines require regular maintenance to ensure optimal performance. When purchasing a machine, consider the availability of accessories such as replacement filters, hoses, and masks. Some suppliers offer packages that include essential accessories, which can simplify the purchasing process. To read more about maintenance click here.
Moreover, consider the ease of cleaning and maintaining the machine. Models with detachable components that are easy to clean can save time and hassle, ensuring that the device remains hygienic and functional.
Price and Budget Considerations
CPAP machines can vary significantly in price, depending on the features and technology included. While it may be tempting to opt for the cheapest option, it is crucial to consider the long-term benefits of investing in a quality machine. A more expensive model may offer advanced features that enhance comfort and effectiveness, ultimately leading to better adherence to therapy.
Insurance and Government Assistance
In Australia, many health insurance plans offer coverage for CPAP machines and related accessories. It is advisable to check with your provider to understand what is covered and whether there are any preferred suppliers. Additionally, the Australian government provides assistance for eligible individuals through the Medical Aids Subsidy Scheme (MASS), which can help offset the cost of purchasing a CPAP machine.
Understanding your financial options can make a significant difference in your purchasing decision. It is worth exploring all available avenues to ensure that you receive the best possible value for your investment.
Warranty and Customer Support
When purchasing a CPAP machine, consider the warranty offered by the manufacturer. A comprehensive warranty can provide peace of mind, ensuring that you are covered in case of defects or issues with the device. Additionally, look for companies that offer robust customer support, as this can be invaluable if you encounter any challenges during setup or use.
Good customer support can also assist with troubleshooting and maintenance queries, making the overall experience smoother and more enjoyable.
Conclusion
Investing time into researching and selecting the right CPAP machine is crucial for effective management of sleep apnoea. With the right device, individuals can experience significant improvements in their sleep patterns, leading to better health outcomes and an enhanced quality of life.
Ultimately, consulting with healthcare professionals and taking advantage of trial opportunities can aid in finding the perfect match for your needs. With the right CPAP machine, restful nights and rejuvenated mornings are well within reach.